
Lameness Evaluation
The lameness of a horse is one of the most common problems that an equine practitioner is called upon to treat. Veterinarians use a systematic approach during the course of an exam so that it is more likely that an accurate diagnosis is made. Careful observation, thorough examination, and persistence are necessary in working up many lameness problems. Some problems can be diagnosed in a few minutes from the history and clinical examination; others require diagnostic local anesthesia (nerve blocks) and several hours of evaluation to determine the source of the lameness.
History, Signalment, And Use
Examination of the horse for lameness begins with a thorough and accurate history. The history can be as important as the clinical signs in leading one to a diagnosis, and this is especially true for difficult or obscure lameness problems. The signalment (age, breed, sex) of a horse is also very important, as many causes of lameness are more common in a certain age of horse or a certain breed of horse. For example, a young horse with joint effusion (extra fluid in a joint) is likely to have an osteochondrosis (OC) lesion, whereas an aged horse with joint effusion is more likely to have osteoarthritis or a traumatic joint injury.
The use or discipline of a horse is a vital part of the history, as many lamenesses result from the type of athletic work that the horse performs. A racehorse is going to have specific common lameness issues related to the work they do, compared to lameness issues common to a dressage horse or a rope horse, for example.
Characterizing the lameness is also important. How long has the lameness been present? How severe has it been? Is the lameness intermittent or constant? Has the lameness been improving or getting worse? Does the lameness improve or become worse with exercise? Does the horse improve on phenylbutazone? Has the horse been rested in a stall, continued in work, or turned out? When did the horse last train or race? Was the horse non-weight bearing on the leg at any time? Has there been heat or swelling in the leg? These types of questions are necessary to obtain a mental picture of the horse’s lameness prior to the examination. For example, a horse that came up acutely lame during a barrel race may be more likely to have a bone bruise or a tendon injury. Whereas, a horse that has been off and on mildly lame for a few months and improves as the horse is warmed up may be more likely to have osteoarthritis in a joint that is slowly progressing.
Recognition Of Lameness
The first step in any lameness examination is to correctly identify the lame limb(s). This requires good powers of observation and experience watching horses move. Normal horses move with balance and bilateral symmetry; they land with equal concussion and move with equal stride length on both the fore and the rear limbs when they are compared side-to-side at a trot. Variation in the normal gait occurs when horses experience pain during movement, have neurologic deficits that affect proprioception and strength, or have a mechanical problem that limits limb use.
Although there are a few gait abnormalities in horses that are mechanical (do not have pain associated with them), most changes in gait are a response to pain. The horse feels pain when it flexes the leg or when weight is transferred across the leg. With most orthopedic problems, pain occurs both during flexion and on concussion when the foot strikes the ground. The horse alters his gait to minimize pain and exhibits gait changes that we recognize as lameness.
Because the horse experiences pain every time the limb is used, lameness gaits are typically consistent and repeated every stride as the horse moves. Therefore, lameness gaits are typically regularly irregular; the horse lands with decreased concussion or shortens his stride the same amount with every step. Mechanical gait abnormalities also tend to be consistent and repeated with every stride, although there is more variation with mechanical gait problems than with lameness.
Neurologic gait deficits, on the other hand, are very inconsistent and these horses tend to be irregularly irregular. Their foot flight, length of stride, and concussion may all vary with each stride. The concept of irregularly irregular is an important one. Neurologic problems are common in horses and the resulting gait abnormalities can be easily confused with lameness. Some horses have both neurologic gait deficits and lameness, making it even more difficult for the examiner to identify the problem. Thorough and careful observation is essential to sorting out the cause of the horse’s abnormal gait.
Lameness examination should always include evaluating the horse at both a walk and a trot, and sometimes at the lope/canter, and/or under saddle, and/or performing in their respective discipline. Most lameness problems are easier to see when the horse is worked at the trot because it is a 2-beat symmetrical gait that makes changes in concussion or stride length easier to observe. In addition, the faster speed of the trot, compared to the walk, increases the stress on the horse’s limb and typically exacerbates the lameness.
 In the front limbs, the horse takes weight off of the affected leg and carries more weight on the sound(er) leg and this body motion is often transferred to head motion. The head can be thought of as a weight that is up on the lame leg and down on the sound (or less lame leg); this results in an observable head nod. It is typically easiest to observe the down movement of the horse’s head, neck, and body as the horse absorbs the concussion of increased weight bearing on the sound limb. This is because some horses with subtle front limb lameness do not have an obvious head nod and do not have an upward movement of the head. In these horses, the examiner observes the increased concussion through the shoulder, neck, and leg as the horse lands on the sound limb and absorbs the increased concussion in his/her whole body. On hard surfaces, the lameness can be heard as well as seen because the foot of the sound leg makes a louder sound as it contacts the ground. Some lameness problems cause the horse pain as the affected limb is advanced forward; this results in a shortened stride and subsequent lower arc of foot flight. The horse may not flex the leg normally and will swing the leg out or in to avoid the normal action required to break squarely over the toe.
In the front limbs, the horse takes weight off of the affected leg and carries more weight on the sound(er) leg and this body motion is often transferred to head motion. The head can be thought of as a weight that is up on the lame leg and down on the sound (or less lame leg); this results in an observable head nod. It is typically easiest to observe the down movement of the horse’s head, neck, and body as the horse absorbs the concussion of increased weight bearing on the sound limb. This is because some horses with subtle front limb lameness do not have an obvious head nod and do not have an upward movement of the head. In these horses, the examiner observes the increased concussion through the shoulder, neck, and leg as the horse lands on the sound limb and absorbs the increased concussion in his/her whole body. On hard surfaces, the lameness can be heard as well as seen because the foot of the sound leg makes a louder sound as it contacts the ground. Some lameness problems cause the horse pain as the affected limb is advanced forward; this results in a shortened stride and subsequent lower arc of foot flight. The horse may not flex the leg normally and will swing the leg out or in to avoid the normal action required to break squarely over the toe.
Hind limb lamenesses are more difficult for the inexperienced eye to see. The horse that is lame behind will land heavier on the sound limb and will unweight the painful (lame) limb. In some horses, uneven concussion between hind limbs results in a “hip hike” where the horse’s hind end stays higher when the lame leg hits the ground and goes down more when the sound leg hits due to the horse taking more weight on the sound limb. This is observed when watching the tail head or the top of the pelvis as the horse trots. More often, you will see the pelvis “move down” when the sound limb is on the ground/as the lame limb comes off the ground. This can be observed by watching over the top of the pelvis. Differences in concussion can also be seen by watching the fetlocks; the fetlock typically drops lower on the sound leg and the horse also spends more time on the sound leg. Thus, the fetlock will drop less on the lame leg because the horse is taking less total weight on that leg. These gait abnormalities give the horse the appearance of “hopping” off of the lame leg onto the sound leg, especially with more obvious/severe lamenesses.
Hind limb lameness is frequently characterized by a shortened anterior phase of the stride (the lame limb is not carried as far forward as the opposite limb) and sometimes a toe drag as the limb is advanced. This is the result of pain on flexion of the limb where the horse will alter his gait to minimize flexion. When the horse is very lame in the hind limb, there may be also be a head nod present which can make it look like it’s a front limb lameness. Horses with moderate-severe hind limb lameness will take weight off of the lame hind limb when that foot hits the ground and appear to lunge forward onto the opposite front leg as the lame hind limb contacts the ground.
For example: At the trot, a horse with severe right hind limb lameness will be nodding down on the left forelimb; this can be confused with a right front limb lameness.
Some hind limb lameness problems are quite subtle; the lame leg can be found by taking a few minutes to study the horse’s gait to determine which foot the horse is landing on with the most force by observing the above-mentioned changes.
Lameness Evaluation

Lameness evaluation begins with observing the horse at rest, standing quietly if possible. It is important to see how the horse chooses to stand, but then to also have the horse stand as square (all feet on the corners of an imaginary rectangle) as possible so you can assess side-to-side symmetry. During this initial phase of the exam, any swellings on the horse’s legs, enlarged joints, or abnormalities in conformation can often be observed without touching the horse. Palpation of the limbs, neck and back can be done before or after the motion exam; this is based on the preference of the veterinarian. Hooftester evaluation also needs to be performed, and this can be done before or after the motion exam; again, based on the preference of the veterinarian. The horse is then evaluated for gait deficits, first at a walk and then at a moderate, steady trot. It is very important to evaluate the horse on smooth, firm ground if possible and to keep the horse’s speed moderate and steady to decrease variations in gait caused by external factors, particularly if the lameness is mild or subtle. Evaluation of the horse for lameness is not always easy, especially if multiple limbs are involved or if the lameness is subtle.
The lameness evaluation should also involve trotting the horse in circles, as this will often exacerbate a baseline lameness or may produce a lameness that was not present in a straight line. Circling often makes the lameness on the inside limb more noticeable, although occasionally lameness on the outside limb is made worse by circling the horse. When the horse is worked in circles, strain is increased on the lateral side of the inside leg and the medial side of the outside leg. In some horses, lameness is not exacerbated by circling, or not present on baseline evaluation, and the horse will need to be ridden under saddle or evaluated while it is performing in its respective discipline.
Once a baseline lameness evaluation is complete, and the limb(s) of interest has been identified, flexions of upper and lower limbs are typically performed. Flexion tests are used to exacerbate baseline lameness or to exacerbate a painful issue that was not visible on baseline evaluation. This is a subjective evaluation and horses of different ages can respond differently. Veterinarians use these tests to add additional information to their baseline lameness evaluation. Following the baseline lameness evaluation and flexions tests, nerve and/or joint blocks are often used to help localize the lameness to the part of the limb that is painful. Nerve and joint blocks involve injecting local anesthetic solution around nerves or into a joint to numb the pain if it is coming from that area. The location of the pain is identified based on the location of the nerve or joint block that improves the lameness. It is always preferred to have an accurate diagnosis so that treatment recommendations are focused on the specific cause of lameness in each individual horse.
For example, if a horse does not block to a foot nerve block, but blocks to a fetlock nerve or joint block, radiographs of the horse’s fetlock would be performed to determine if there was any bone abnormality visible on the radiographs. If radiographs were normal, an ultrasound evaluation of the fetlock region could be done to look at soft tissue structures around the fetlock. Furthermore, if no cause of the lameness was found with radiograph and ultrasound evaluation of the fetlock, magnetic resonance imaging may be recommended to perform a more in-depth evaluation of the bone and soft tissue structures in the horse’s fetlock.
Case Example
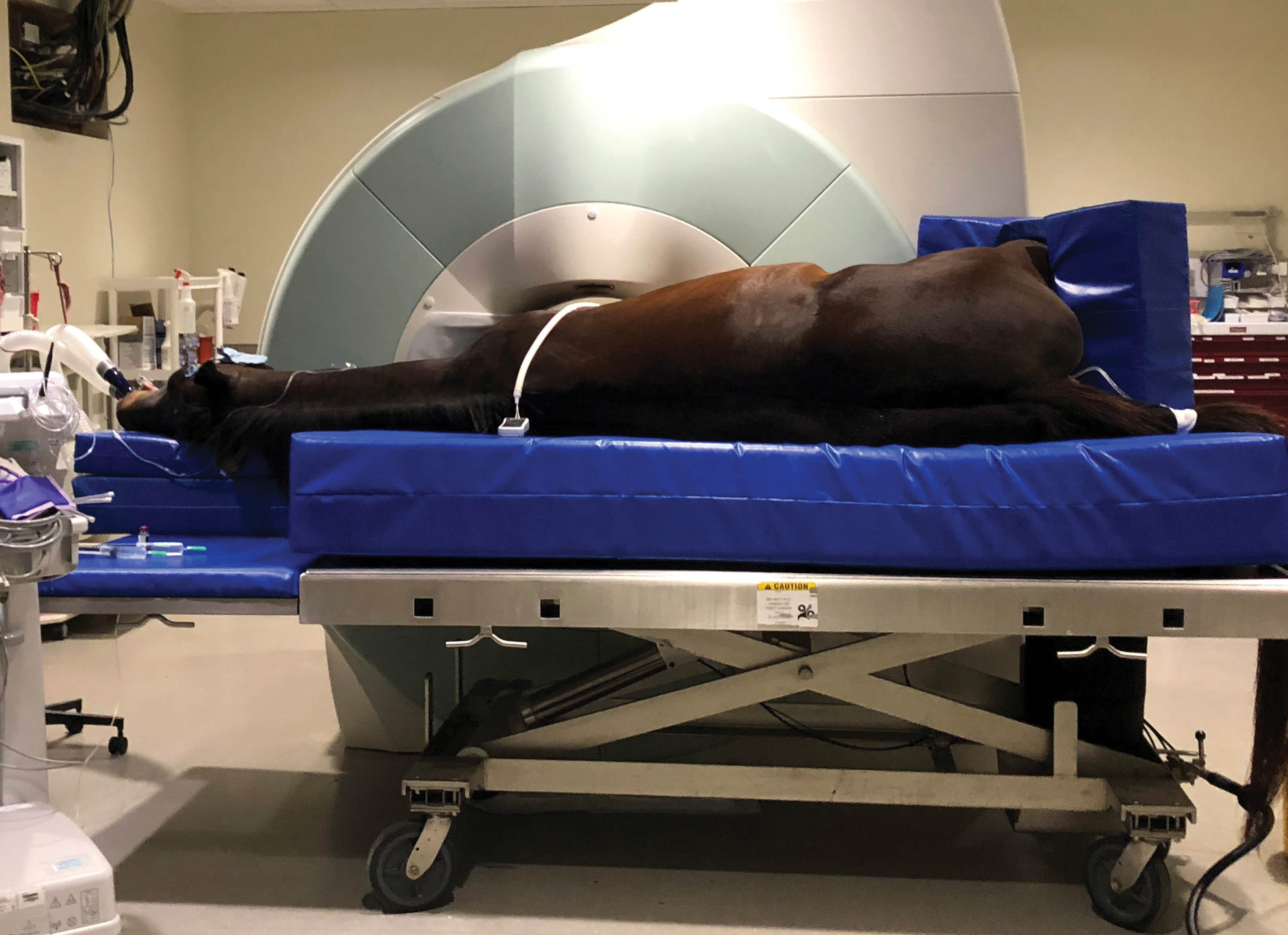 A 10-year-old Quarter Horse gelding used for barrel racing presented for a hindlimb lameness that was recently identified. The horse had a consistent right hind lameness in a straight line and circling both directions, but the cause of the lameness was unknown. There was no obvious swelling of the limb. The horse was more positive to upper limb flexions tests than he was to lower limb flexion tests. A decision was made to block the horse’s two lower hock joints because hock pain can be a common cause of lameness in western performance horses. After the joint block was performed, the horse was significantly less lame in the right hind limb. The joint block had taken away at least 70% of the pain in the limb and, therefore, the area that was causing the lameness was identified. However, we still did not know the cause of the pain. Radiographs were then taken of the right hock, but there was no injury visible to any bones of the hock. The next diagnostic step to more completely evaluate the bones and soft tissue structures of the hock was magnetic resonance imaging (MRI). This horse then had an MRI evaluation done on the right hock and a non-displaced, complete fracture of the central tarsal bone was identified. Now that we had a definitive diagnosis of the cause of the horse’s pain, treatment could be instituted to give this horse the best chance to return to performance. The horse was then taken to surgery to put two lag screws through the tarsal bone fracture. The horse was rested for 3 months and then was able to return to a conditioning program to prepare the horse to return to competition.
A 10-year-old Quarter Horse gelding used for barrel racing presented for a hindlimb lameness that was recently identified. The horse had a consistent right hind lameness in a straight line and circling both directions, but the cause of the lameness was unknown. There was no obvious swelling of the limb. The horse was more positive to upper limb flexions tests than he was to lower limb flexion tests. A decision was made to block the horse’s two lower hock joints because hock pain can be a common cause of lameness in western performance horses. After the joint block was performed, the horse was significantly less lame in the right hind limb. The joint block had taken away at least 70% of the pain in the limb and, therefore, the area that was causing the lameness was identified. However, we still did not know the cause of the pain. Radiographs were then taken of the right hock, but there was no injury visible to any bones of the hock. The next diagnostic step to more completely evaluate the bones and soft tissue structures of the hock was magnetic resonance imaging (MRI). This horse then had an MRI evaluation done on the right hock and a non-displaced, complete fracture of the central tarsal bone was identified. Now that we had a definitive diagnosis of the cause of the horse’s pain, treatment could be instituted to give this horse the best chance to return to performance. The horse was then taken to surgery to put two lag screws through the tarsal bone fracture. The horse was rested for 3 months and then was able to return to a conditioning program to prepare the horse to return to competition.
